Since January 1, 2017, Medicare has reimbursed physicians and other health care professionals for providing comprehensive care planning to individuals with a cognitive impairment - a critical step in improving the quality of care and quality of life for those with Alzheimer's and their caregivers. A care planning visit includes an evaluation of cognition and function, measuring neuropsychiatric symptoms, a safety evaluation, identifying and assessing a primary caregiver, development of advance care directives, and referrals to community services.
The bottom line is that care planning helps ensure those with Alzheimer's get on the right care path. And, analyses show getting on the right care path reduces costs to Medicare as a result of fewer emergency department visits, fewer hospitalizations, and better medication management. This is why the Alzheimer's Association and Alzheimer's Impact Movement (AIM) fought for years to enact the HOPE for Alzheimer's Act, and why we were pleased to see the Centers for Medicare and Medicaid Services (CMS) create a new care planning benefit for cognitively impaired individuals in Medicare.
But are people using it? Are they taking advantage of what care planning can do to improve quality of care and quality of life? Do they even know the benefit exists?
To answer those questions, the Alzheimer's Association and AIM contracted with the Health Care Cost Institute (HCCI) to analyze the use of the care planning benefit among Medicare fee-for-service (FFS) beneficiaries and among those in some Medicare Advantage (MA) plans. The results show that, unfortunately, very few Medicare beneficiaries received care planning in 2017, the first year it was available:
- 18,669 FFS Medicare beneficiaries received care planning, a rate of 55.6 per 100,000 beneficiaries.
- 2,857 individuals in the Medicare Advantage plans that were analyzed* received the benefit, a rate of 39.4 per 100,000 beneficiaries.
- In seven states and Washington, D.C., not a single FFS Medicare beneficiary received the care planning benefit.

At the end of the day, fewer than one percent of those living with Alzheimer's and other dementias received care planning in 2017.
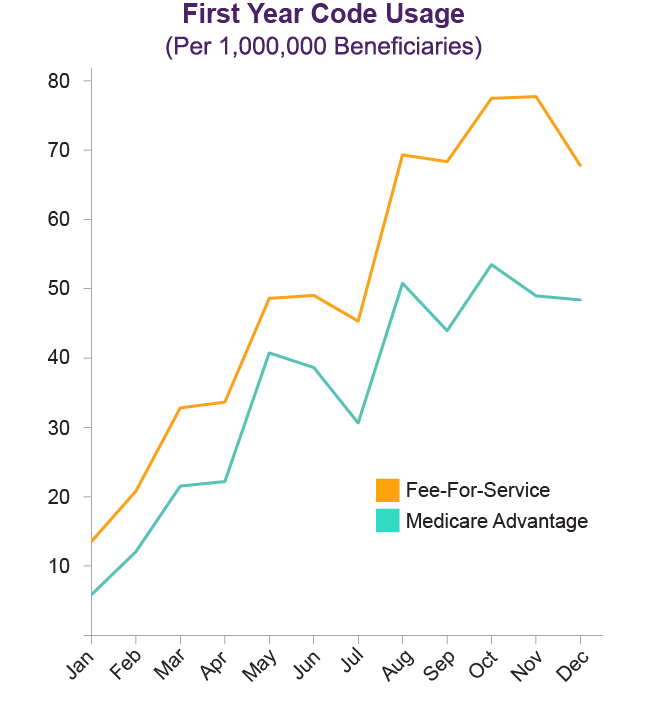
The good news is that as more people and providers become aware of the benefit, the more it is used. In 2017, the number of people who received care planning steadily increased over the course of the year. In January, fewer than 500 people received the benefit, but in December, more than 2,000 did. Use of the code was more than three times greater in the fourth quarter of the year than the first quarter (3.3 times in FFS plans and 3.8 times in MA plans).
It is clear that in order for the benefits of care planning to reach more Americans affected by Alzheimer's, more awareness of the care planning benefit is needed. The Improving HOPE for Alzheimer's Act (S. 880/H.R. 1873) would address this very issue. The legislation builds on the care planning benefit by requiring the Department of Health and Human Services to (1) educate clinicians on the existence and importance of Medicare's care planning benefit; and (2) report to Congress on the barriers to individuals receiving care planning services and how use of the benefit can be increased.
As Congress adjourned for its August recess, the Improving HOPE for Alzheimer's Act had already garnered significant bipartisan support. The House bill (H.R. 1873) has 76 cosponsors, and the Senate bill (S. 880) has 39. More support, however, is needed. Contact your member of Congress to ask him or her to sign on today.
In the absence of a treatment that would change the underlying course of the disease, we must do all we can to ensure the best quality of care and quality of life for those living with Alzheimer's. Care planning is a key linchpin in that effort.
________________________*The Medicare Advantage plans analyzed represented 37 percent of total enrollment in Medicare Advantage plans.