By now, many have heard the exciting news out of Texas. On Nov. 4, 2025, Texas voters overwhelmingly approved Proposition 14, authorizing $3 billion over 10 years to fund the Dementia Prevention and Research Institute of Texas (DPRIT) — the largest state-funded dementia research initiative in the nation. It was a landmark moment, and the Alzheimer's Association and AIM were proud to play a central role in making it happen.
But Texas is not the only state making history in the fight against Alzheimer’s and other dementia. Across the country, state lawmakers are stepping up in a meaningful way.
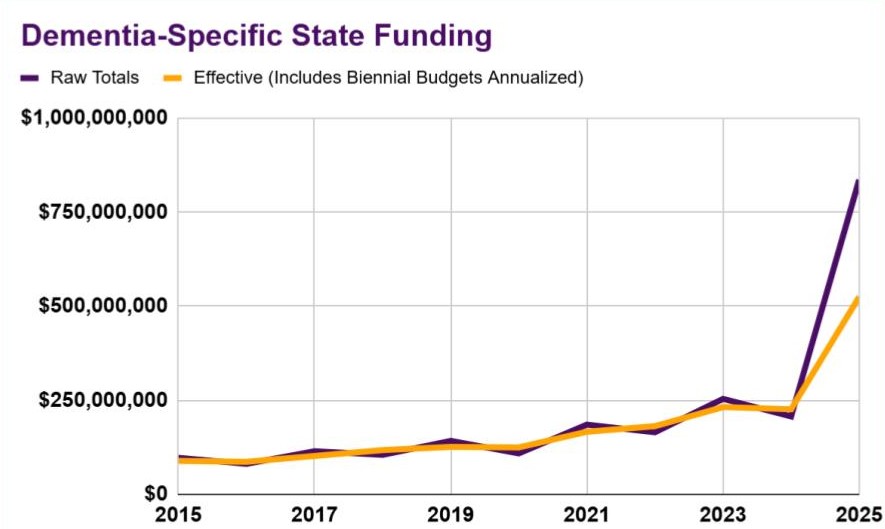
Beyond Texas, states across the country dedicated hundreds of millions of dollars to dementia research, caregiver support, public awareness, workforce development and more. This breadth of investment reflects years of persistent, bipartisan advocacy by AIM’s nationwide network of volunteer advocates — and a growing recognition that dementia is a public health crisis that demands state action.
Importantly, dementia-specific state appropriations are not one-size-fits-all. They reflect each state’s priorities and the diverse needs of people living with dementia and their families — from research initiatives to caregiver respite programs, care specialist networks, dementia registries and public education campaigns.
Advancing Dementia Research
Several states made significant investments in dementia research this year. Beyond DPRIT, Florida appropriated $87.358 million in dementia-specific funding — including $5 million to the Ed and Ethel Moore Alzheimer’s Disease Research Program, $3 million for ultrasound-based Alzheimer’s research and $5 million to University of Florida Health for Alzheimer’s and dementia research. Mississippi directed $3 million to Alzheimer’s research. Arizona appropriated $4.125 million for Alzheimer’s research funding, and Colorado invested $500,000 in dementia-specific research.
Supporting Caregivers Through Respite
Family caregivers are the backbone of dementia care in this country, and states are increasingly recognizing the need to support them with respite care. Caregiving takes a significant physical and emotional toll, with 74% of dementia caregivers saying that they are concerned about maintaining their own health since becoming a caregiver. Respite care provides caregivers a temporary rest from caregiving, while the person living with dementia continues to receive care in a safe environment.
Ohio appropriated $4.3 million for Alzheimer’s-specific respite care. Missouri dedicated $1.55 million to dementia-specific respite care. West Virginia appropriated more than $2.3 million for the Roger Tompkins Alzheimer’s Respite Care Program. South Carolina invested $900,000 for dementia-specific respite care. Connecticut appropriated $1.8 million to support its Statewide Respite Care Program, and Maine invested $566,057 in its State Respite Care Program.
Building a Dementia Care Workforce
A number of states focused on ensuring that care workers, health providers and community members have the knowledge and tools to support people living with dementia. Indiana invested $1.425 million annually through the biennium in its Dementia Care Specialist program to increase community awareness, improve access to resources and provide training. Louisiana appropriated $824,000 to establish and expand its Dementia Care Specialist program statewide across its nine Adult and Disability Resources Centers. Georgia invested $1.25 million to fund a Dementia Care Specialist program with one staff position in each of the state’s 12 Area Agencies on Aging. Hawaii dedicated $525,000 to establish two full-time positions to coordinate and integrate dementia training into existing University of Hawaii programs and develop a dementia curriculum to build an informed dementia workforce.
Building Infrastructure and Improving Care
States also made strategic investments in the infrastructure needed to address dementia over the long term. Pennsylvania appropriated $1.9 million to fund the creation of an Alzheimer's Disease and Related Dementias Office in the Pennsylvania Department of Aging. Maryland invested $2.4 million to fund long-term care and dementia care navigation within the Department of Aging. New York appropriated nearly $36.7 million, spanning Alzheimer's disease care and service infrastructure, research assistance, community service programs and a Special Needs Assisted Living Residential Voucher for People with Dementia program. Wisconsin appropriated nearly $16 million, including more than $9.2 million over the biennium for its statewide Dementia Care Specialist program and $6.1 million for the Alzheimer’s Family and Caregiver Support Program.
As treatments advance and the population ages, the pressure on state health care systems, Medicaid budgets and families will only grow. When states dedicate funding to address dementia, they signal that this is a public health priority. By building infrastructure that will outlast any single legislative session, states across the nation are creating real, tangible support for families who cannot wait.
Behind every appropriation on this list is a volunteer advocate — someone living with dementia, a family caregiver, a health care professional — who showed up, shared their story and urged their state lawmakers to act. AIM’s passionate advocates have spent years building the relationships and bipartisan support that make progress like this possible. AIM will continue working with advocates and bipartisan champions in all 50 states to ensure state governments are taking action to support people affected by Alzheimer’s and all other dementia.
To learn more about state dementia policy priorities — or to get involved as an advocate in your state — visit alzimpact.org/state.
